Chesterfield mums share ‘terrifying’ experiences of the life-threatening illness their kids suffer after having Covid
and live on Freeview channel 276
Paediatric Inflammatory Multisystem Syndrome, or PIMS, is an illness which develops in some children around four-six weeks after having Covid-19. It causes inflammation throughout the body, and is thought to occur when the immune system overreacts to having to fight off Covid.
The main symptom is a persistent high temperature, but others include a rash, stomach pains, muscle aches, red and cracked lips, headaches, swollen neck glands, diarrhoea and vomiting.
Advertisement
Hide AdAdvertisement
Hide AdThe illness is treatable, but the inflammation may affect the blood vessels around the heart, which can be life-threatening if not addressed.


Sarah Morris said her seven-year-old son Samuel started to show symptoms about a month after testing positive for Covid. He had a high temperature along with severe back and abdominal pain, but staff at an out-of-hours service said Samuel was suffering from a virus and sent him home.
Sarah said: “He then got very poorly - he could barely stand, we had to carry him upstairs, he developed a rash all over his body and tongue, and he was squealing with the pain in his back. He was being sick and had diarrhoea, and it got to the point where we knew it couldn’t be viral, it had to be more than that.
“We took him to A&E, they did several tests and put him down as having scarlet fever, and his temperature was hitting 40. Luckily, a doctor looked over his notes during the night, and because she knew about PIMS, she put the pieces together and diagnosed that.”
Advertisement
Hide AdAdvertisement
Hide AdSamuel was then rushed to an intensive care unit at Sheffield Children’s Hospital, where he received treatment for PIMS. Although he is now out of hospital and improving, Samuel has suffered damage to his heart, and Sarah said that too many medical staff lack awareness and understanding of the illness.

“He’s getting better, but he has got some damage to his heart as a result of PIMS, and possibly, because of how long it took to diagnose. We’re going to Leeds next week for an appointment with a cardiologist to see what the state of his heart is and the next steps.
“It’s been traumatic. We are starting to hope that there is some light at the end of the tunnel, but he was off school yesterday because he was absolutely shattered. It just seems to be a never-ending nightmare really, it's terrifying.
“The main thing we’re finding is that frontline healthcare providers don't know enough about it - your GPs, certain A&E nurses and doctors, as well as 111 call handlers. It’s the same thread over and over again.”
Advertisement
Hide AdAdvertisement
Hide AdFor Ganga Gnanaraj, the story is much the same. Her 11-year-old son Shenan was sent home twice from A&E despite having symptoms of PIMS, with one doctor misdiagnosing him with tonsillitis.

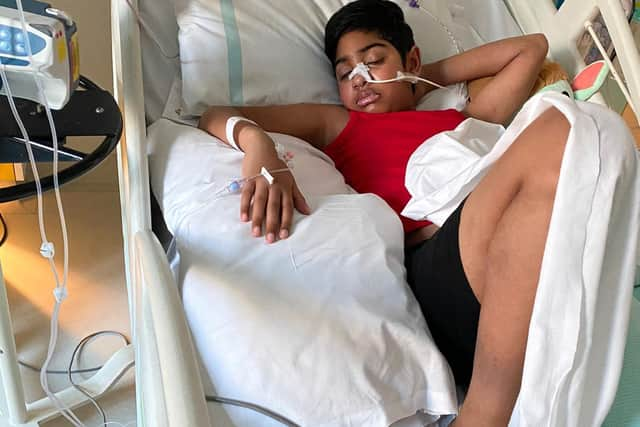
It was only when Shenan was struggling to breathe and hallucinating that he was admitted at Chesterfield Royal Hospital, having also developed a huge lump on his neck.
Ganga said: “The people at A&E couldn’t understand why he had been sent home twice. They realised he was really poorly, but they thought he had lymphangitis because of the lump on his neck.
“Two of my friends know Sarah, and they sent me a post that she had put on Facebook about PIMS and what had happened to Samuel. I asked the doctor if it could be PIMS, and they asked me who told me about that, before saying that they weren't sure, but would talk to a paediatrician.”
Advertisement
Hide AdAdvertisement
Hide AdAnother paediatrician assessed Shenan and realised that Ganga was right, but by this stage, Shenan’s condition had deteriorated drastically, and doctors were unsure whether he would survive.


Ganga said: “They told me he only had a 50/50 chance because it was that bad, and they sent him to the ICU at Sheffield. I had to ring Shenan’s dad to come in to see him - it was really, really bad.
“We were there in Sheffield for two weeks and they were giving him the maximum dose of everything they could. They were using the Great Ormond Street guidance for PIMS, but they said his case was unlike anything they had seen before, because they just couldn't get the temperature down.
“They had to do a surgery through his throat on the lump on his neck, so he was being tube fed after that - he couldn’t talk, he couldn’t eat anything. Shenan was really suffering for so many days, and his echocardiogram showed he now has a leaky valve on his heart, and his coronary artery is not good.
Advertisement
Hide AdAdvertisement
Hide Ad“My GP asked where Shenan was at an appointment the other day, and I told her he’d had PIMS, and she asked me what that was - none of them had heard of it.”
Megan Allfree took her son Theo, 6, to the Royal with a high temperature and rash.
“We took him to the Royal and they put it down to a tummy bug.


“We then noticed the bloodshot eyes, which we obviously knew wasn’t normal. Luckily, the A&E doctor the second time we went took one look at Theo and said it looked like Kawasaki, which is a similarly-linked syndrome.”
Advertisement
Hide AdAdvertisement
Hide AdTheo’s quick diagnosis was crucial in ensuring that his heart did not sustain any lasting damage, but Megan said she was concerned about scenarios like Ganga’s, where parents are directing medical staff as to what their children may be suffering from.
“We see a lot of people who say their doctors aren't aware of it and palm you off with something else. On a Facebook group for parents of kids with PIMS, one poor child had his appendix taken out and it eventually turned out to be PIMS.
“Trust your own instincts. GPs, doctors and nurses might say it’s a tummy bug or whatever, but all three of us as mums put our foot down and said something wasn’t right. It is really worrying that parents are having to tell doctors what it could be.
“How can healthcare professionals not be clued up on it? There’s stuff about meningitis everywhere, everyone knows what to look for with that, so why aren’t we doing the same with PIMS?”
Advertisement
Hide AdAdvertisement
Hide AdThe three mums are now sharing their stories to raise awareness of PIMS amongst other parents and carers, as well as frontline medical staff. Sarah said that it was crucial for PIMS to be diagnosed as early as possible, and urged parents to make themselves aware of the symptoms and to ask doctors to consider it when treating their children.
“It’s time critical- the faster you can get the steroids into the child to stop the inflammation, the better chance they’ve got of a quicker recovery and not having lasting heart damage.
“If your kids have got a high temperature and one or two of the other symptoms, don’t mess around- take them to A&E and tell them that you think it’s PIMS, and you want them to do the blood work and the echo scan.
“Parents, carers and frontline workers need to know the signs and symptoms of PIMS- it is incredibly rare, but it is incredibly real, and it can be life-threatening.”
Advertisement
Hide AdAdvertisement
Hide AdDr Hal Spencer, Medical Director at Chesterfield Royal Hospital NHS Foundation Trust, said: “The clinical impact – not forgetting the emotional impact – of COVID continue to emerge and develop across all healthcare settings. We continue to learn and proactively respond to situations such as this and can confirm that we are teaching on this regularly.
"Thankfully, this is an extremely rare condition, and children who are affected and are treated here at the Trust will continue to receive the best possible care – in line with national best practice.
“We are continually improving our training, education and awareness and this will ensure cases are identified and managed appropriately. We wish all the children and their families well and would encourage everybody to ensure they are up-to-date with any available vaccines, as this remains the best course of action for many to protect infection.”
More information on PIMS, including a full list of symptoms, can be found here.
Advertisement
Hide AdAdvertisement
Hide Ad